Tele-Anesthesia and Remote Monitoring: The Future of Anesthesia Care is Virtual
The digital transformation that has reshaped commerce, communication, and entertainment is now profoundly altering the landscape of medicine. Anesthesia, a specialty at the intersection of advanced technology, physiology, and patient safety, is at the forefront of this change. The convergence of high-speed networking, sophisticated sensors, and artificial intelligence has given rise to two interconnected concepts: Tele-Anesthesia and Remote Monitoring. Together, they promise to revolutionize perioperative care by expanding access to expertise, enhancing patient safety, and creating a more efficient and resilient healthcare system.
This is not about replacing the hands-on anesthesiologist but about augmenting their reach and capabilities, creating a new paradigm of collaborative, technology-enhanced care.
Part 1: Defining the Core Concepts
While often used together, it's crucial to understand that tele-anesthesia and remote monitoring are two distinct components of a larger system.
What is Tele-Anesthesia?
Tele-anesthesia is the delivery of anesthesia care and expertise from a distance, using telecommunications technology. It is the "human" element of the remote equation, encompassing several key applications:

Pre-operative Assessment: A patient in a rural or distant clinic can have a comprehensive pre-anesthesia evaluation via a secure video conference. The remote anesthesiologist can review the patient's electronic health records (EHR), discuss their medical history, and order necessary tests, all before the patient even travels to the hospital.
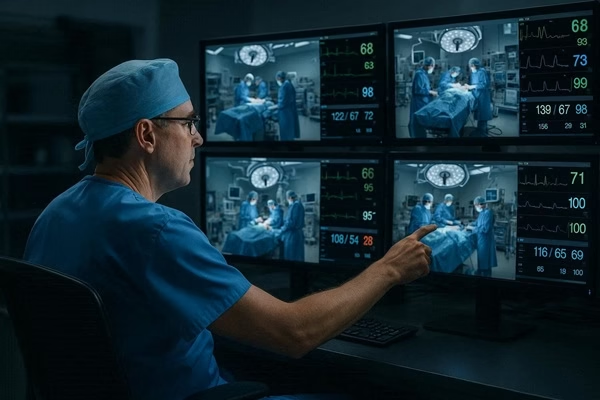
Intra-operative Support (The "Anesthesia Command Center"): This is the most transformative application. A senior anesthesiologist or a team of them sits in a central "command center," monitoring real-time data from multiple operating rooms in different hospitals. They provide oversight, guidance, and support to on-site anesthetists, residents, or non-physician anesthesia providers. This is particularly valuable for:
- Rural Hospitals: Providing access to specialist expertise for complex cases.
- Ambulatory Surgery Centers (ASCs): Allowing a single supervising anesthesiologist to oversee multiple rooms simultaneously.
- Emergency Support: Providing immediate virtual consultation in critical situations.
Post-operative and Critical Care Rounds: After surgery, anesthesiologists can remotely check on patients in the Post-Anesthesia Care Unit (PACU) or the Intensive Care Unit (ICU), review their vitals and labs, and communicate with the on-site nursing staff to manage pain, nausea, and other complications.
What is Remote Monitoring?
Remote monitoring is the technological backbone that makes tele-anesthesia effective. It involves the continuous, automated collection and transmission of patient physiological data to a central location where it can be analyzed and acted upon.
- Advanced Bedside Monitors: Modern OR monitors transmit high-fidelity waveforms (ECG, blood pressure, SpO2, EtCO2) in real-time.
- Wearable Biosensors: For pre- and post-operative wards, lightweight, wireless patches can continuously monitor vital signs like heart rate, respiratory rate, and oxygen saturation, allowing for early detection of deterioration on a general floor.
- Integration with AI and Machine Learning: This is where remote monitoring becomes truly powerful. Algorithms can analyze vast streams of data to identify patterns and predict adverse events before they become critical. For example, an AI might flag a subtle trend in a patient's vital signs that predicts an impending episode of hypotension, allowing the remote anesthesiologist to proactively intervene.
Part 2: The Synergy in Action: A Typical Workflow
Imagine a patient undergoing a general surgery in a small, rural hospital.
- Pre-op: The patient has a tele-anesthesia consultation with a specialist at a regional medical center.
- Intra-op: The on-site Certified Registered Nurse Anesthetist (CRNA) administers the anesthesia. Simultaneously, all of the patient's real-time vital signs and data are streamed to a command center 200 miles away.
- The Alert: An AI-powered monitoring system detects that the patient's end-tidal CO2 is rising and their blood pressure is beginning to trend downwards—a subtle but potentially ominous sign.
- The Intervention: An alert pops up on the screen of the remote anesthesiologist. She immediately brings up the video feed to the OR, assesses the surgical field, and speaks directly to the CRNA through a headset. "I see a trend toward hypoventilation and developing hypotension. Let's reduce the anesthetic vapor concentration and give a small fluid bolus. I'm pulling up the chart now to check for any other factors."
- The Outcome: The potential crisis is averted before it fully develops. The patient remains stable, thanks to the combination of intelligent monitoring and immediate expert oversight.
Part 3: Key Benefits and Driving Forces
The adoption of tele-anesthesia is accelerating due to its compelling advantages.
- Enhanced Patient Safety: Continuous expert oversight and AI-driven predictive analytics create a powerful safety net, catching issues that might be missed by a busy provider focused on a single task.
- Democratization of Expertise: It allows smaller or underserved hospitals to offer a level of surgical care that was previously only available at major academic centers, bridging the gap in healthcare access.
- Increased Efficiency and Cost-Effectiveness: A single anesthesiologist can provide supervision for multiple operating rooms, optimizing staffing models and reducing the need for travel between sites.
- Support for Junior Staff: It serves as an invaluable educational tool and a safety net for anesthesiology residents and early-career providers, giving them access to mentorship in real-time.
- Public Health Resilience: The COVID-19 pandemic was a massive catalyst. Tele-anesthesia allowed for the conservation of PPE, protected vulnerable staff by minimizing physical contact, and ensured continuity of care when staffing was limited.
Part 4: Challenges and Hurdles to Adoption
Despite its promise, the path to widespread implementation is not without significant challenges.
- Technological Infrastructure: The system is entirely dependent on reliable, high-speed internet and robust, secure networks. Any lag or outage could be catastrophic.
- Legal and Regulatory Licensure: Medicine is licensed at the state level in the U.S. A physician in California cannot easily provide care to a patient in Nevada. Clear national and international telehealth licensure compacts are needed.
- Data Security and Privacy: Transmitting sensitive patient data requires ironclad security measures to prevent breaches and maintain compliance with regulations like HIPAA.
- Human Factors and Team Dynamics: Building trust and effective communication between the remote anesthesiologist and the on-site team is critical. The on-site provider must feel supported, not micromanaged.
- Emergency Response: The most significant clinical hurdle. A remote anesthesiologist cannot perform a life-saving emergency intubation or insert a central line. The system is only as good as the competence and training of the person physically present with the patient.
Part 5: The Future Outlook
The future of tele-anesthesia and remote monitoring is incredibly bright and will be shaped by further technological integration.
- Augmented Reality (AR): Imagine a remote specialist being able to see exactly what the on-site provider sees through AR glasses, and even project instructions or anatomical overlays into their field of view to guide a difficult procedure.
- Fully Integrated Closed-Loop Systems: The ultimate goal is a "closed-loop" system where an AI, under the supervision of a remote human expert, can automatically adjust drug infusions to maintain a patient's physiological parameters within a desired range.
- Expansion Beyond the OR: The principles of remote monitoring and expert oversight will be applied to entire hospital wards, creating "virtual ICUs" that monitor all patients for signs of deterioration.
Conclusion
Tele-anesthesia and remote monitoring are not a futuristic fantasy; they are a present-day reality that is rapidly redefining the practice of anesthesia. By leveraging technology to extend the eyes, ears, and expertise of the anesthesiologist, this model creates a collaborative ecosystem of care. It promises a future where geography is no longer a barrier to top-tier medical care, where data is used to predict and prevent harm, and where every patient, no matter where they are, can benefit from the watchful eye of a specialist. This is the dawn of a more connected, intelligent, and safer era in perioperative medicine.