Anesthesia Machine & Anesthesia Workstation
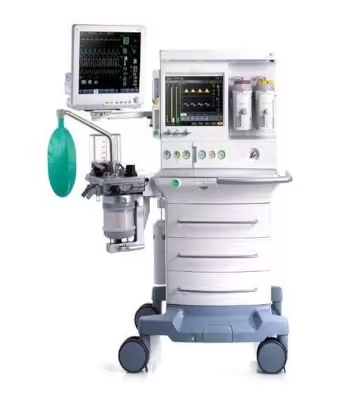 Welcome to the nerve center of the operating room. The anesthesia workstation, with its complex array of dials, circuits, and monitors, can seem like an intimidating beast. But what if you could master it? This comprehensive resource is your guide on a fascinating journey—from the historic, clunky elegance of the Boyle's machine to the sleek, intelligent workstations of Dräger, GE, and Mindray that define modern practice. We will demystify the physics, deconstruct the components, and build your confidence. This isn't just about learning a machine; it's about understanding your most critical partner in ensuring patient safety.
Welcome to the nerve center of the operating room. The anesthesia workstation, with its complex array of dials, circuits, and monitors, can seem like an intimidating beast. But what if you could master it? This comprehensive resource is your guide on a fascinating journey—from the historic, clunky elegance of the Boyle's machine to the sleek, intelligent workstations of Dräger, GE, and Mindray that define modern practice. We will demystify the physics, deconstruct the components, and build your confidence. This isn't just about learning a machine; it's about understanding your most critical partner in ensuring patient safety.
Our journey will be a methodical one. We'll start by laying a strong foundation, exploring the history and the core physics that govern every machine. From there, we'll build up your knowledge piece by piece, dissecting the classic anatomy of an anesthesia machine and mastering the circle breathing system. Only then will we leap into the modern era, comparing the sophisticated features of today's leading workstations. Each module is designed to build upon the last, transforming a daunting subject into a clear, manageable, and ultimately, masterable skill.
Fiberoptic Intubation
Fiberoptic intubation is the cornerstone of managing the anticipated difficult airway. By visualizing the glottis without aligning oral, pharyngeal, or laryngeal axes, it enables awake or anesthetized intubation. Mastery requires deliberate practice, topical anesthesia skills, and a clear backup plan.
Supraglottic Airway Placement
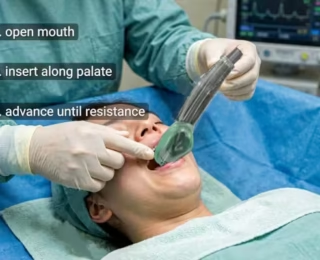
The supraglottic airway (SGA) sits above the glottis, providing rapid, hemodynamically stable ventilation for short, low‑risk cases. Master LMA and i‑gel insertion, cuff management, and troubleshooting leaks or obstruction. SGAs are critical rescue devices in “cannot intubate, cannot ventilate” scenarios. Never use with a full stomach.
Endotracheal Intubation
Endotracheal intubation (ETI) is the cornerstone of modern airway management in anesthesia. It involves placing a flexible plastic tube into the trachea to secure the airway, permit positive pressure ventilation, protect against aspiration, and deliver inhaled anesthetics. For the anesthesia trainee, mastering ETI is not merely a technical skill—it is the first major step toward becoming a competent perioperative physician.
Intravenous Regional Anesthesia (Bier Block)
The Bier Block provides rapid, bloodless anesthesia for distal limb procedures lasting under 60 minutes. This guide covers indications, double-tourniquet safety, 0.5% lidocaine dosing (no epinephrine), and the critical 20-minute minimum inflation rule. Master IVRA to safely avoid local anesthetic systemic toxicity while optimizing surgical conditions.
Peripheral Nerve Blocks
Peripheral nerve blocks are essential for targeted perioperative analgesia, reducing opioids and enhancing recovery. This guide covers sonoanatomy, local anesthetic pharmacology, common upper/lower extremity blocks, complications like LAST, and evidence-based techniques. Ideal for trainees mastering ultrasound-guided regional anesthesia from basics to advanced clinical practice.
Levosimendan
Levosimendan is a calcium sensitizer and KATP channel opener that increases contractility without raising intracellular calcium or myocardial oxygen demand. Its active metabolite lasts ~80 hours. Ideal for low cardiac output with renal failure (no dose adjustment) or when milrinone fails. Key risks: hypotension and prolonged effects.
Milrinone
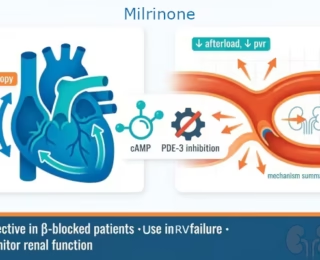
Milrinone is a PDE-3 inhibitor used in cardiac anesthesia as an inodilator—it increases contractility while reducing afterload and pulmonary vascular resistance. Ideal for right ventricular failure and β-blocked patients. Key risks: hypotension and prolonged half-life in renal failure. Avoid bolus if hypotensive or hypovolemic.
Mephentermine
Mephentermine is an indirect sympathomimetic that releases endogenous norepinephrine, increasing both heart rate (β-1) and SVR (α-1). Ideal for spinal-induced hypotension with bradycardia or low cardiac output. Longer-acting than ephedrine but risks tachyphylaxis. Avoid in tachycardic or ischemic patients.
Disclaimer!
The information provided on this platform, including but not limited to articles, case studies, clinical scenarios, guidelines, and multimedia content, is intended for educational and informational purposes only.
The authors and editors of this material have made every effort to ensure the accuracy of treatments, drugs, and dosage regimens that conform to currently accepted standards. However, due to continual changes in information resulting from ongoing research and clinical experience, unique aspects of individual clinical situations, as well as the potential for human error; readers must exercise personal judgment when making a clinical decision.
This website may contain third-party information or links to other internet websites. We do not control nor assume responsibility for any third-party content provided nor content on linked Internet websites.
We strongly recommend the visitors of this website to go through its Detailed 'Disclaimer' and 'Terms of Use'.
By accessing, browsing, or using this website, you acknowledge that you have read, understood, and agreed to be bound by the 'Disclaimer' and 'Terms of Use'. If you do not agree with these terms, you must NOT use this website.