Introduction: What is a BIS Monitor and Why is it Needed?
A Bispectral Index (BIS) Monitor is a neurophysiological monitoring device that provides a quantifiable measure of a patient's level of consciousness. It is most commonly used during general anesthesia and procedural sedation to help clinicians titrate anesthetic drugs.
The fundamental challenge in anesthesia is that it is a "black box" state. Unlike blood pressure or heart rate, there is no simple, direct way to measure if a patient is truly unconscious. Traditional signs like movement or autonomic responses (heart rate, blood pressure) are unreliable indicators of awareness.
The BIS monitor was developed to solve this problem by translating the complex electrical activity of the brain into a single, easy-to-understand number. Its primary goals are to:
- Prevent Intraoperative Awareness: Reduce the risk of a patient being conscious during surgery.
- Avoid Over-Sedation: Prevent administering excessive anesthetic drugs, which can lead to delayed wake-up, hemodynamic instability (low blood pressure), and potential side effects.
The Technology: How Does BIS Work?
The BIS monitor is a type of processed EEG (Electroencephalogram) monitor. Here’s a step-by-step breakdown of its technology:
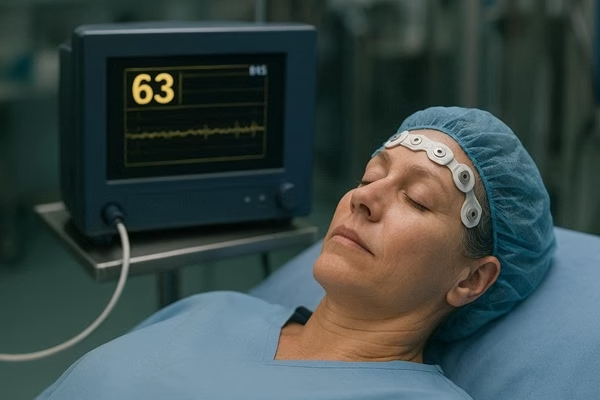
Signal Acquisition: A disposable BIS sensor, placed on the patient's forehead, contains electrodes that pick up the raw electrical signals from the brain's cortex (the EEG).
The Problem with Raw EEG: A raw EEG tracing is extremely complex, full of noise, and requires a trained neurologist to interpret. It is not practical for an anesthesiologist to use in real-time during surgery.
The BIS Algorithm: The core of the technology is a sophisticated, proprietary algorithm that analyzes the raw EEG signal. It performs several key analyses:
- Bispectral Analysis: This is the "secret sauce" and the source of the name "Bispectral." The algorithm doesn't just look at the power of brainwaves at different frequencies; it analyzes the phase relationships (or "phase coupling") between them. When the brain is in a deep, synchronized state (like deep sleep or anesthesia), different brainwave frequencies are more phase-locked. When awake, they are more random and desynchronized. This analysis is highly sensitive to changes in the hypnotic state.
- Burst Suppression Analysis: At very deep levels of anesthesia, the brain's activity can become intermittent, with periods of electrical silence (suppression) punctuated by brief bursts of activity. The algorithm detects and quantifies this pattern.
- EMG (Electromyography) Analysis: The algorithm also measures the level of high-frequency activity from muscle (EMG), which can interfere with the EEG signal.
The Output: The algorithm integrates all these complex analyses into a single number: the BIS Value, which ranges from 0 to 100.
The Hardware Components
- BIS Sensor: A single-use, flexible strip with 3 or 4 electrodes that is applied to the patient's forehead. The electrodes are impregnated with a conductive gel and are designed for easy application and good signal quality. There are specific sensors for adults and pediatric patients.
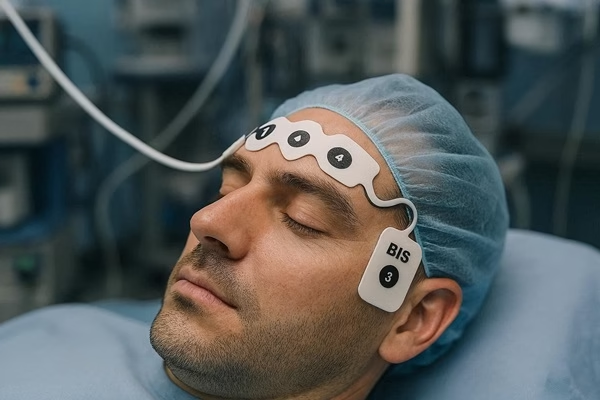
- BIS Monitor: The processing unit that connects to the sensor. It can be a standalone bedside monitor or, more commonly, a module integrated into a larger multi-parameter patient monitor (e.g., GE Healthcare, Philips, Medtronic). The screen displays the BIS value, the raw EEG waveform, the Signal Quality Index (SQI), and an EMG bar.
Interpretation: What Do the Numbers and Displays Mean?
Understanding the display is crucial for using the monitor effectively.
BIS Value | Patient State | Clinical Interpretation |
|---|---|---|
| 90 - 100 | Awake | The patient is fully conscious and alert. |
| 70 - 90 | Light Sedation | The patient is drowsy but can be easily aroused. |
| 60 - 70 | General Anesthesia | This is the typical target range for most surgeries. The patient is unconscious. |
| 40 - 60 | Deep Hypnosis | A deeper level of unconsciousness. May be appropriate for certain procedures but increases risk of burst suppression. |
| < 40 | Very Deep Anesthesia | Approaching burst suppression. Generally avoided unless clinically indicated. |
| 0 | Flat EEG | No brain electrical activity. |
Other Key On-Screen Elements:
- EEG Waveform: Shows the raw brain activity, allowing the clinician to visually inspect for artifacts or specific patterns.
- Signal Quality Index (SQI): A percentage (0-100%) indicating the quality of the EEG signal. A low SQI (e.g., < 50%) means the BIS value may be unreliable due to poor electrode contact or electrical interference.
- EMG Bar: Indicates the level of muscle activity. High EMG (from shivering, patient movement, or teeth grinding) can contaminate the EEG signal and falsely elevate the BIS value, making the patient appear more awake than they are.
Clinical Applications
- Operating Room (OR):
- Titration of Hypnotics: The primary use is to guide the administration of intravenous hypnotics like propofol and volatile anesthetic gases (sevoflurane, desflurane). The goal is to maintain the BIS within the 40-60 range, adjusting drug infusion rates accordingly.
- Facilitating "Fast-Track" Surgery: By avoiding over-sedation, patients wake up more quickly and clearly, which can speed up recovery and discharge from the post-anesthesia care unit (PACU).
- Intensive Care Unit (ICU):
- Sedation Management: Used to titrate sedative infusions (e.g., propofol) for mechanically ventilated patients, ensuring they are adequately sedated but not oversedated, which can prolong ventilation.
- Procedural Sedation:
- Used for procedures like endoscopy, interventional radiology, or cardiac electrophysiology, where a moderate level of sedation is required.
Advantages and Limitations
Advantages:
- Objective Measure: Provides a data-driven, objective measure of hypnosis, reducing guesswork.
- Reduces Awareness: Numerous studies have shown that BIS-guided anesthesia significantly reduces the incidence of intraoperative awareness.
- Improved Efficiency: Leads to faster wake-up times and reduced anesthetic drug consumption.
- Ease of Use: The sensor is simple to apply, and the number is easy to interpret.
Limitations:
- It is NOT a "Depth of Anesthesia" Monitor: This is the most important distinction. BIS only measures the hypnotic component of anesthesia. It does not measure analgesia (pain relief) or immobility (muscle relaxation). A patient can have a low BIS value (be unconscious) but still have a strong stress response to surgical pain.
- Artifacts and Interference: The signal can be corrupted by electrocautery, pacemakers, patient movement, or high EMG activity, leading to inaccurate readings.
- Unreliable with Certain Drugs: Ketamine and nitrous oxide (N2O) produce EEG patterns that the BIS algorithm does not interpret well, often leading to falsely high values.
- Patient-Specific Factors: The BIS value can be less reliable in patients with neurological disorders (e.g., dementia, brain injury) or in the very young or very old.
- Delay: There is an inherent 10-30 second delay between a change in the patient's brain state and its reflection in the BIS value.
Conclusion
The Bispectral Index (BIS) monitor has become a standard tool in modern anesthesia and critical care. By providing a window into the brain's hypnotic state, it has empowered clinicians to deliver more precise, individualized, and safer care. It has been instrumental in reducing the devastating complication of intraoperative awareness while also promoting faster patient recovery.
However, it is crucial to remember that the BIS monitor is an adjunct, not a replacement for clinical judgment. An anesthesiologist must integrate the BIS value with a comprehensive assessment of the patient, including hemodynamic data, surgical stimuli, and their own clinical experience. It is one piece of a complex puzzle, but an invaluable one at that.