The Syringe Infusion Pump: A Masterclass for Anesthesia Providers
In the intensive care units (ICUs) as well in the operating room, the syringe infusion pump is as essential as the laryngoscope. While it appears to be a simple device—a motor pushing a syringe—it is our primary tool for precision drug delivery. For anesthesia residents, mastering the pump is not just about programming numbers; it is about understanding pharmacokinetics, patient safety, and crisis management.
This guide will cover the mechanics, clinical applications, safety pitfalls, and advanced troubleshooting of the syringe driver.
1. The Basics: How It Works
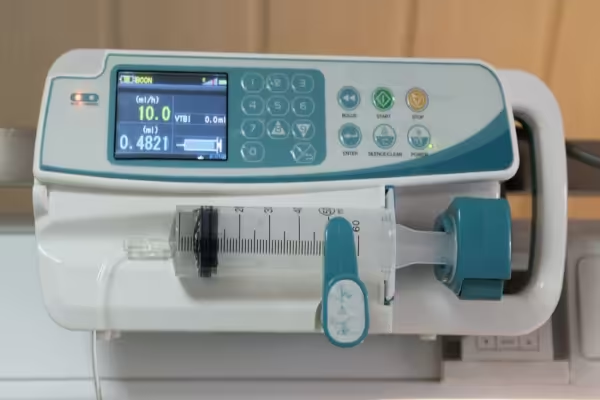
A syringe infusion pump delivers fluids at a programmed rate (mL/hr) by applying mechanical force to the plunger of a syringe.
Mechanism:
A stepper motor drives a lead screw, which pushes a pusher block against the syringe plunger.
Components:
Syringe Holder: Clamps the barrel.
Pusher Block: Moves the plunger.
Drive Mechanism: The motor and screw assembly.
User Interface: Keypad and display for rate, volume, and drug selection.
Alarms: Occlusion, near-empty, battery low, air-in-line (less common in syringe pumps vs. volumetric pumps, but present in advanced models).
2. Clinical Applications in Anesthesia
We use syringe pumps primarily for continuous infusions where precise titration is required.
| Drug Class | Common Examples | Why a Pump? |
|---|---|---|
| Vasopressors | Norepinephrine, Phenylephrine, Vasopressin | To maintain hemodynamic stability with minute-to-minute titration. Bolus errors can be catastrophic. |
| Inotropes | Dobutamine, Milrinone | Precise cardiac output management. |
| Sedatives | Propofol, Dexmedetomidine (Precedex) | To achieve targeted sedation scores (e.g., RASS) and TCI (Target Controlled Infusion) if available. |
| Muscle Relaxants | Cisatracurium, Rocuronium | To maintain a steady state for surgical conditions. |
| Induction Agents | (Rarely) Ketamine, Remifentanil | Ultra-short acting agents for total intravenous anesthesia (TIVA). |
3. The "Resident’s Checklist": Setup and Programming
Errors in pump setup are a leading cause of intraoperative medication errors. Follow this checklist every time:
A. Syringe Selection
Compliance matters: A 50 mL syringe is stiffer than a 20 mL syringe. Always tell the pump what size syringe you are using. If the pump thinks a 20 mL syringe is a 50 mL one, it will under-deliver volume (or over-deliver pressure) significantly.
Brand compatibility: If the pump has a setting for "BD" vs "Terumo," select it. The external diameter varies by manufacturer, affecting the clamp fit.
B. Priming
Never connect before priming. Always disconnect the syringe from the extension line, prime the line (including the dead space) until fluid exits the distal end, then connect to the patient.
Why? If you prime after connection, you deliver a bolus of the drug (especially dangerous with vasopressors).
C. Loading
Ensure the plunger is properly seated in the pusher block.
Perform the "Occlusion Test" : Start the pump against a clamped line briefly to ensure the alarm triggers. This verifies the pressure sensor works.
D. Programming
Double-check the concentration. Is it mcg/mL? mg/mL?
Check the rate. Use the "Rate" vs "Dose" calculation features if the pump offers drug library software (smart pumps).
4. Physics & Safety: Occlusion Pressure
One of the most critical concepts for trainees is Occlusion Pressure and Post-Occlusion Bolus.
Because syringe pumps push against a fixed volume, if the line becomes kinked (occlusion), pressure builds up in the syringe and tubing.
The Problem: When the occlusion is suddenly released (e.g., you unkink the line or open a clamped stopcock), the stored potential energy is released, delivering a bolus of the drug instantly.
Magnitude: This bolus can be up to 0.5 mL to 2.0 mL, depending on the:
Syringe size: Smaller syringes = higher pressure for same force.
Tubing length: Long, compliant tubing = larger potential bolus.
Flow rate: Low flow rates (e.g., 1 mL/hr) are the most dangerous because the pump takes longer to alarm, allowing pressure to build higher.
5. Smart Pumps and Drug Libraries
Modern anesthesia relies on "Smart Pumps" equipped with Drug Libraries (e.g., Alaris Guardrails, B. Braun DoseTrac).
Soft Limits: The pump warns you if you enter a dose above the recommended range, but allows you to override.
Hard Limits: The pump prevents administration of a dose above the safety threshold.
Trainee Tip: Do not ignore soft limits. If you are overriding them, you should be able to verbally justify why to your attending (e.g., "This patient is extremely vasoplegic; I need to exceed the standard limit transiently").
6. Common Alarm Scenarios & Troubleshooting
| Alarm | Likely Cause | Action |
|---|---|---|
| Occlusion | Kinked line, closed stopcock, clot in catheter, patient position. | 1. Disconnect from patient. 2. Release line to expel bolus into a gauze. 3. Reconnect. Never simply "silence" and restart. |
| Syringe Empty | Infusion complete. | Prepare a new syringe. Use a syringe swap technique (if pump allows) to avoid interruption. If not, disconnect, change, prime, reconnect. |
| Low Battery | Unplugged from mains. | Plug it in. Never rely on battery for a long case. Battery runtime is for transport only. |
| Drive Disengaged | Pusher block moved away from plunger during transport. | Re-engage drive mechanism; ensure plunger is seated against pusher; restart infusion. |
| Air in Line | (If equipped) Air bubbles in extension set. | Disconnect, purge air, reconnect. |
7. Advanced: Total Intravenous Anesthesia (TIVA) and TCI
For residents learning TIVA, the syringe pump is the centerpiece.
Context-Sensitive Half-Time: Unlike inhalational agents, IV drugs accumulate in peripheral compartments. The pump allows you to manage this.
Target Controlled Infusion (TCI): (Available outside the US in some devices, or via specific platforms). TCI uses pharmacokinetic models (e.g., Marsh, Schnider) to calculate a rate to achieve a target plasma or effect-site concentration. While TCI improves ease of use, the anesthesiologist must still understand the model limitations (e.g., obesity, elderly, cardiac output).
8. Safety Summary: Pearls for Residents
Label everything: Use color-coded syringe labels (e.g., red for vasopressors, blue for sedatives). A naked syringe looks like a syringe of saline—until it isn't.
Trace lines: Follow the line from the pump to the patient. Ensure you aren’t infusing norepinephrine into a stopcock port that is closed.
The "Dead Space" Hazard: When using multi-lumen central lines, the dead space of the lumen (approx. 1.2–1.5 mL) acts as a reservoir. If you stop a vasopressor, it takes several minutes for the drug in the dead space to clear.
Weight entry: If your pump calculates dose based on weight (mcg/kg/min), ensure the weight is correct and updated post-induction if the patient was weighed on the bed.